Under what circumstances should lymphoma patients undergo "genetic testing" to maximize its value and save costs?
In the last lesson, we discussed the types and functions of "genetic testing" for lymphoma. Click the text to read the previous content: What types of "genetic testing" are available for lymphoma patients? What are their respective functions?
Now, for such an expensive test, when is the best time to do it to "maximize its value and save treatment costs"?
A very good question!
Below, I will share with you the most valuable timing for "genetic testing":
1. At the time of initial diagnosis:
First situation—Genetic testing must be done:
When lymphoma is first diagnosed, if the pathological diagnosis has certain doubts and the pathology report suggests genetic testing to assist in confirming the diagnosis, it is crucial to follow the pathologist’s recommendation for the related genetic tests. This is the only way to definitively diagnose lymphoma and its subtype, allowing for appropriate treatment.Second situation—Genetic testing is recommended:
If the pathological diagnosis is very clear, we suggest that patients with the financial means may opt for genetic testing.The image below shows lymphoma clustering based on next-generation genetic sequencing results by foreign scholars. It further divides the three subtypes from the previous COO classification into seven subtypes. Over 60% of large B-cell lymphomas can be categorized into a specific subtype, while around 30% cannot be clustered. Performing genetic clustering analysis on large B-cell lymphoma can guide doctors in selecting targeted therapeutic drugs.
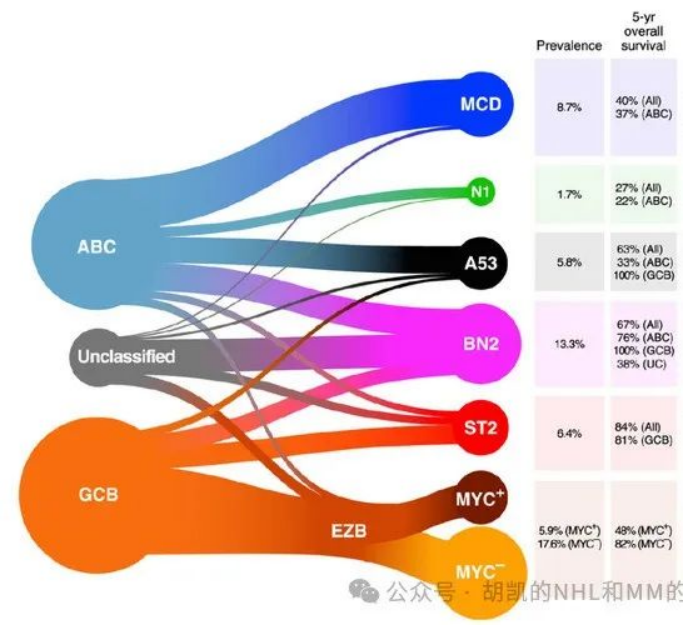
The image is from the academic literature
Reason:
Firstly, although the first-line standardized treatment for lymphoma is based on pathological classification, the guiding value of genetic testing results for the standard treatment plan in newly diagnosed patients is still under exploration. However, some studies suggest that based on genetic testing results, combining targeted drugs with the standard treatment regimen may lead to better efficacy.
For example, diffuse large B-cell lymphoma of the MCD or BN2 subtype may benefit from the R-CHOP regimen combined with BTK inhibitors, etc.Secondly, for newly diagnosed patients, while the first-line standard treatment might be the same regardless of genetic testing results, knowing the genetic characteristics could potentially assist in choosing the overall treatment strategy.
For example, if high-risk mutations such as MYC or TP53 mutations are present, there may be a heightened concern for chemotherapy resistance, and adjustments to the treatment plan may be necessary. This information could also help in deciding whether to proceed with autologous stem cell transplantation later on.
2. When "refractory" or "relapsed" status occurs:
What is "refractory"?
It refers to a situation where after receiving "2 cycles" of "standard full-dose first-line chemotherapy," the patient has not achieved "partial remission (PR)."What is "relapsed"?
It refers to the condition where, after the disease has achieved "remission," lesions reappear with an increase in size or the emergence of new lesions.When either of these two situations occurs, it is strongly recommended to perform second-generation genetic testing!
On one hand, it helps to understand the reasons for tumor resistance and what high-risk genetic characteristics may have contributed to the poor treatment response.
On the other hand, there is no unified standard treatment plan for relapsed or refractory cases. At this point, precise individualized treatment needs to be selected. Therefore, the results of genetic testing are essential in guiding drug selection to improve the success rate of salvage therapy.
3. After treatment remission or completion of treatment:
At this stage, treatment has been concluded, and the most concerning and worrisome question is whether the disease will relapse.
Usually, regular follow-up PET/CT or contrast-enhanced CT scans are used to monitor whether the disease has maintained complete remission.
However, since PET or CT scans cannot be performed too frequently, typically only every three months or even every six months, there is always a possibility of disease relapse or progression during the gap between scans.In recent years, blood tests to monitor tumor-related ctDNA (as discussed in the previous lesson) have provided new technical methods for disease monitoring. Therefore, during remission, it is recommended to monitor peripheral blood ctDNA to detect early relapse.
However, it is important to note that a single ctDNA positive result does not always clearly indicate relapse. Continuous dynamic monitoring over a period of time is often needed to provide more valuable and meaningful insights.
Expert Introduction

















